16 Mar Can Diabetes Cause Swelling in Feet? Causes, Symptoms & What to Do
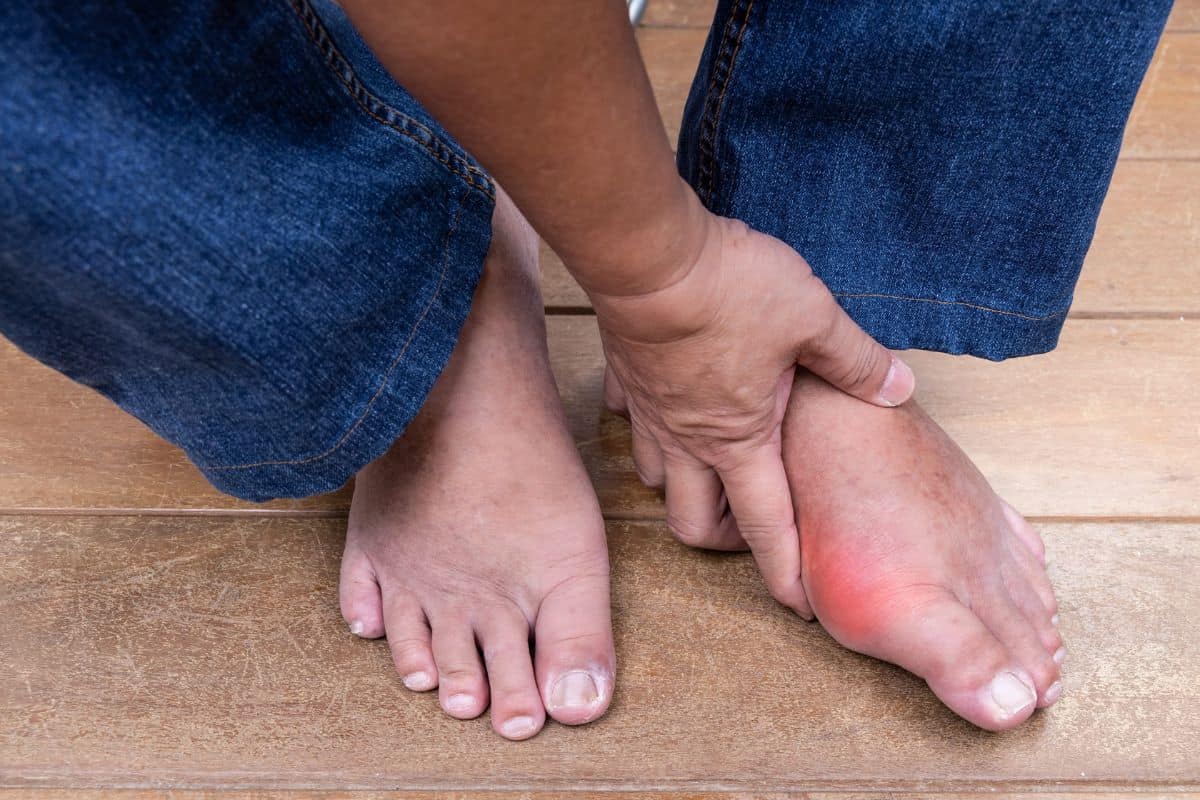
If you’re wondering can diabetes cause swelling in feet, you may notice your feet look puffier than usual, feel tight in shoes, or leave an indentation when pressed. For the millions of Americans living with diabetes, swollen feet are not just a cosmetic annoyance—they are a warning signal that demands your attention.
So, can diabetes cause swelling in the feet? The short answer is yes—and in multiple ways. Diabetes affects your circulatory system, nerves, kidneys, and lymphatic system, all of which play a role in how your body manages fluid. Understanding why your feet are swelling, what it means, and what you can do about it could literally save your limbs and your life.
At Winds of Change in Muskogee, OK, we specialize in exactly this kind of care. Our founder, Lynette Gunn, APRN, CNS, has spent over 18 years treating lower extremity conditions—and she’s here to walk you through everything you need to know.
Can Diabetes Cause Swelling in Feet? Here’s the Science
Yes—diabetes can and does cause swelling in the feet, and it does so through several overlapping mechanisms. This condition is known medically as peripheral edema. and in people with diabetes, it is rarely caused by just one factor. Instead, it tends to result from a cascade of physiological changes that build on one another over time.
Here is how each system plays a role:
1. Poor Circulation (Peripheral Arterial Disease)
High blood sugar damages the walls of blood vessels, making them stiff, narrow, and less efficient. When blood struggles to flow effectively through your legs and feet, fluid can leak from the vessel walls and pool in surrounding tissues. The result? Swelling, heaviness, and discoloration—especially in the lower extremities.
2. Diabetic Neuropathy
Diabetes is the leading cause of peripheral neuropathy in the United States. When nerves in the legs and feet are damaged, the blood vessels they help regulate lose their tone and may dilate abnormally, allowing more fluid to seep into tissue. Neuropathy also reduces your ability to feel pain, which means injuries and infections—each of which causes swelling—can go undetected for longer.
3. Diabetic Kidney Disease (Nephropathy)
Your kidneys filter waste from your blood and help regulate fluid balance. In people with longstanding diabetes, the kidneys begin to lose their filtering efficiency. When protein leaks into the urine (a condition called proteinuria) and the kidneys retain sodium and water, fluid accumulates in the tissues—often first noticed in the feet and ankles.
4. Venous Insufficiency
Damaged vein valves in the legs can no longer push blood back up toward the heart efficiently. Gravity does what gravity does—blood and fluid pool at the lowest point, which is your feet. People with diabetes are at increased risk for venous insufficiency, particularly if they are also overweight, sedentary, or have a history of blood clots.
5. Medication Side Effects
Certain medications commonly prescribed to people with diabetes—including some calcium channel blockers for blood pressure and thiazolidinediones for blood sugar—list foot and ankle swelling as a known side effect. If your swelling began after starting a new medication, this connection is worth discussing with your provider.
Warning Signs You Should Never Ignore
Swelling alone is concerning enough. But when combined with any of the following symptoms, it becomes urgent. Do not wait for your next scheduled appointment if you experience:
- Swelling that is warm, red, or painful to the touch
- Skin that appears shiny, stretched, or discolored
- An open sore, blister, or wound on or between the toes
- A foul odor coming from the foot, even without a visible wound
- Swelling that appears suddenly in only one foot
- Fever or chills alongside foot swelling
- Numbness, tingling, or burning sensations that are worsening
Any wound or sore on a diabetic foot can rapidly escalate into a serious infection. Diabetic foot ulcers are the leading cause of non-traumatic lower limb amputations in the United States. Catching problems early changes outcomes dramatically.
Ready to take control of your foot health? Call us today or visit our website to schedule your appointment. Specialized care is closer than you think.
How Diabetic Foot Swelling Is Diagnosed
When you come to Winds of Change, your evaluation is never rushed. Lynette Gunn takes a comprehensive, whole-person approach to understanding the causes of your swelling. A thorough assessment may include:
- A complete review of your medical history, current medications, and blood sugar control patterns
- Physical examination of both feet and lower legs, including skin integrity, temperature, color, and pulses
- Monofilament testing to assess nerve sensitivity and detect early neuropathy
- Ankle-brachial index (ABI) to screen for arterial insufficiency.
- Wound assessment and measurement to determine if any ulceration or skin breakdown is present
- Referral coordination with your primary care provider or specialist if systemic issues, such as kidney or cardiac involvement, are suspected
This level of detail matters. Many patients with diabetic foot complications have seen multiple providers without ever receiving this kind of thorough evaluation. At Winds of Change, the assessment is not just a formality—it is the foundation of your care plan.
What You Can Do at Home: Practical Steps That Make a Real Difference
While professional care is essential for managing diabetic foot swelling, you can take meaningful action every day. Think of these not as burdensome tasks, but as investments in your mobility and independence:
- Elevate Your Feet Intentionally: When you sit or rest, prop your feet above heart level. Even 20 to 30 minutes a few times per day can significantly reduce fluid pooling in the lower legs and feet.
- Move More, Even Gently: Calf raises, ankle circles, and short walks stimulate the muscle pump in your legs, which helps push blood and lymph back upward. Prolonged sitting or standing in one position worsens edema.
- Inspect Your Feet Daily—Without Exception: Use a hand mirror to examine the bottoms of your feet every evening. Look between the toes. Check for blisters, cuts, cracks, calluses, or any change in skin color. If you notice anything new, document it with a photo and contact your care provider.
- Wear Properly Fitted, Diabetic-Friendly Footwear: Shoes that are too tight restrict circulation and create pressure points that lead to wounds. Diabetic shoes are designed with extra depth and width, seamless interiors, and protective soles. Do not sacrifice function for style when your limbs are at stake.
- Manage Blood Sugar Consistently: Elevated blood glucose is the underlying driver of virtually all the complications discussed in this article. Working with your healthcare team to keep your A1C and daily glucose readings in a healthy range reduces your risk of all diabetic foot complications, including edema.
- Reduce Sodium Intake: Sodium causes your body to retain water. Reducing processed foods, canned soups, and restaurant meals can have a noticeable impact on fluid retention within days.
Why Choose Winds of Change
When it comes to diabetic foot care, not all providers are created equal. Wound and foot care is a highly specialized field, and the difference between a generalist and a specialist can mean the difference between healing and amputation.
Here is what sets Winds of Change apart:
- Lynette Gunn brings over 18 years of specialized wound and foot care experience, including her tenure as Chief of Outpatient Nursing at the Eastern Oklahoma VA Health Care System.
- We treat the whole person—not just the wound. Every visit begins with listening, not just examining.
- We serve veterans with deep respect and understanding, knowing that trust must be earned and maintained.
- Our Muskogee, OK, location is designed to be accessible, comfortable, and judgment-free for patients of all backgrounds.
- We offer medical transport and financing options, so cost and logistics do not become barriers to the care you need.
- Lynette also trains the next generation of wound care professionals, which means our practice stays current with the latest evidence-based practices.
Lynette’s guiding philosophy says it best: “I want to journey hand-to-hand with you.” At Winds of Change, you are never just a chart number or a wound to be dressed. You are a person with a story, and we are here to help write the next, healthier chapter.
Conclusion
Diabetic foot swelling is not something to dismiss, delay, or manage alone. It is a sign that your body is working hard against significant internal pressure—and it deserves a thoughtful, expert response.
Now that you know the answer to “can diabetes cause swelling in feet” is a definitive yes—and that the causes run deep and the risks are real—you are equipped to take action. Whether that means adjusting your daily habits, scheduling a foot inspection with a specialist, or finally addressing that wound that has been slow to heal, every step you take matters.
At Winds of Change in Muskogee, OK, we are here when you are ready. Our expertise is real, our care is personal, and our commitment to your health is unwavering. Do not wait for a small problem to become a crisis. Reach out today and take the first step toward healthier feet and a more confident life.
Your feet carry you through life. Let us help carry them. Visit our website or call our office to book your personalized care visit today. You deserve care that is both clinically excellent and genuinely kind.
Frequently Asked Questions
1. Can diabetes cause swelling in the feet even if my blood sugar is controlled?
Yes. Once nerve damage, vascular changes, or kidney dysfunction have developed, swelling can persist even when blood glucose levels are well-managed. However, good blood sugar control significantly slows the progression of these complications and reduces the risk of new swelling developing.
2. Is diabetic foot swelling always painful?
Not necessarily. Because diabetic neuropathy reduces sensation, many patients experience significant swelling without notable pain. This is actually one of the most dangerous aspects of diabetic foot complications—the absence of pain does not mean there is no problem. Regular visual inspection is essential for this reason.
3. How quickly can diabetic foot swelling turn into a serious problem?
Faster than most people expect. A blister caused by swollen feet rubbing against a shoe can develop into an infected ulcer within days in a person with poor circulation and impaired immune response. Any new wound on a diabetic foot warrants prompt professional evaluation, ideally within 24 to 48 hours.
4. Does Winds of Change accept patients who are not veterans?
Absolutely. While Lynette Gunn has deep expertise and personal passion for serving veterans, Winds of Change welcomes all patients in need of specialized wound and foot care. Everyone in the Muskogee, OK area and surrounding communities is welcome to schedule an appointment.
5. What should I bring to my first appointment at Winds of Change?
Bring a list of all current medications (including supplements), your most recent lab results if available, any photos you have taken of your foot or wound over time, a list of questions or concerns, and comfortable clothing that allows easy access to your lower legs and feet. Most importantly, bring yourself—we will handle the rest.


Sorry, the comment form is closed at this time.